RELEVANT BASIC SCIENCE RESEARCH FOR INFERTILITY PRACTICE
Basic bench research is of crucial importance in all medical fields but there is at least one reason why it in infertility is, likely, more important than in most other specialty areas of medicine: Because it usually involves pregnancy, human clinical research in infertility is much more restricted than in any other medical specialty areas. Consequently bench research and animal models assume even greater responsibility for progress that in other medical specialties.
Today’s postings reflect this fact, as they address the growing number of embryo implantation models being developed in laboratories and offering important new information about what still is the most widely used animal model – the mouse – by comparing mouse and human ovaries along advancing ages in both species.
We hope you will enjoy the discussions of both subjects and – as always – want to encourage you to become an active participant by either commenting on our postings or even proposing an article. We also want to take this opportunity to remind you to sign up for a free subscription to the Reproductive Times [HERE] and register at greatly discounted early bird rates for this year’s annual Foundation for Reproductive Medicine Conference (FRMC) in NYC on December 4-6 which the CHR as always co-sponsors [HERE].
Finally, we want to bring to our reader’s attention several new clinical trials which recently were approved by the CHR’s IRB, have been formally registered, and are ready for enrollment. If you or somebody you know may be interested in enrolling, please call the CHR’s registration desk at (212) 994 4400.
The CHR’s Editorial Staff
One of the most basic issues the CHR has been pursuing almost since its establishment in 1981 in Chicago, is the information deficit between clinical practice of infertility and the research bench. What we mean by that is the ignorance of clinical fertility practice about relevant basic research that is going on in research laboratories and the ignorance of research scientists in reproductive biology and other related research areas about how their research could contribute to improvements of clinical practice when it comes to female and male infertility. This has also been the principal reason why the CHR in collaboration with The Foundation for Reproductive Medicine (FRM) established the annual December FRM Conference (FRMC) which – as its principal goal – brings leading basic scientists and clinicians together in one room for three days, so that they can learn what their mutual needs for collaboration are.
As part of this effort, we today – based on several recent publications - are discussing two important basic research areas with significant potential relevance for clinical infertility.
Will Newly Developed Models of Embryo Implantation Finally Allow a Better Understanding of Implantation?
Several laboratories have recently reported workable models for human implantation, raising expectations for a better understanding of the process. One – by Chinese investigators – is still at preprint stage at eLife.1 A second one by European investigators was just published in its full beauty in Cell.2
The first paper claims to have established an endometrial organoid culture system that mimics the window of implantation. Considering that nobody really exactly knows when this alleged implantation window starts and ends in a cycle, it seems to us that the claim of having an endometrial organoid system mimicking the window of implantation may be a little exaggerated. The second paper by a European collaborative established a 3D in vitro model that supposedly “supports” human implantation and development. With what defines a “receptive” endometrium still somewhat controversial, the authors of this paper attempt to define it molecularly.
Implantation of a human embryo into the endometrium is, of course, likely the most crucial event in pregnancy. It, after all, marks the very beginning of a pregnancy. It is also – for a variety of known and probably even more unknown reasons – is prone to high failure rates. Even at peak fertility in the early 20s, only 1/3 embryos will implant. By age 45, this ratio is probably around 1/20.
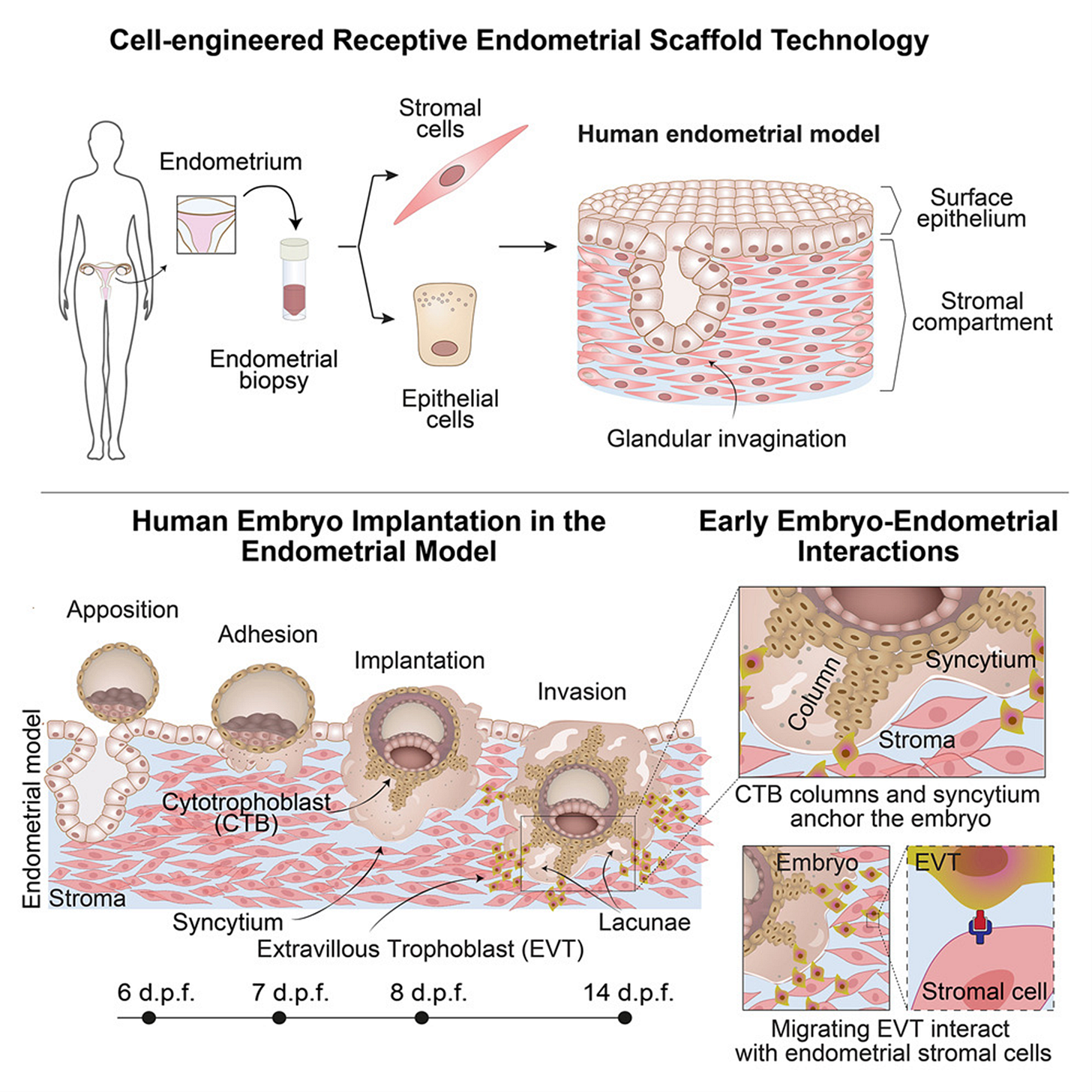
The European model is alleged to recapitulate the luminal, glandular, and stromal compartments of the superficial layer of receptive human endometrium. Human embryos as well as blastoids allegedly implanted into this endometrial model, achieving post-implantation hallmarks including advanced trophoblast structures that underlie early events in placental development.
Single-cell RNA sequencing of the embryo-endometrial interface at day 14 uncovered predicted molecular interactions between conceptus and endometrium. Disrupting signaling interactions between extravillous trophoblast and endometrial stromal cells caused defects in trophoblast outgrowth, demonstrating the importance of crosstalk processes to sustain embryogenesis (see the Graphic Abstract below). This study does offer potentially important insights into our understanding of implantation!
But there is a “but” - and this “but” relates to a subject that on several occasions before has been addressed in these pages , - the question whether pregnancy should primarily be viewed as an endocrine event (i.e., dependent on a hormonal “window of implantation”) or an immune event – first and foremost – dependent on the development of appropriate maternal tolerance toward the fetal semi-allograft (and increasingly full allograft if egg donation or a gestational carrier are involved).
We here, of course, will not rekindle this discussion; but – while not ignoring the relevance of hormones for the establishment of successful implantation and pregnancy, the CHR sees pregnancy, for biological reasons, as primary an immune- rather than endocrine- mediated condition. And this opinion, of course, also translates into clinical practice, which – for decades – has given close attention to our patients’ immune systems.
We, therefore, strongly believe that all the modelling of implantation will remain unsatisfactory until and unless models also receive an “immune system.”
REFERENCES
Zhang et al., eLife 2025. https://doi.org/10.7554/eLife.90729.3
Molè et al., Cell 2026;189:1-19
Comparing human and mouse ovaries across advancing ages
Though mouse models have been used in ovarian research for decades, - neither women nor men are mice.” We here at the CHR learned this a long-time ago, even-though it was mouse work by colleagues which, finally, explained to us ( and whoever was interested in knowing) why androgen supplementation (in our case with DHEA) in hypo-androgenic women often improves outcomes in IVF cycles.1 Considering how especially difficult in vivo human research can be in the fertility field, without obtaining these mouse data we still might not understand why androgen supplementation (including with DHEA) is so successfully in treating hypo-androgenic infertile women with androgen supplementation in preparation for IVF.
But because neither women nor men are mice, not everything observed in mice will also end up applying to the human experience. We, therefore, were intrigued when colleagues from UCSF recently published a paper in Science comparing mouse and human ovaries over advancing ages2 (the Graphic Abstract is below).
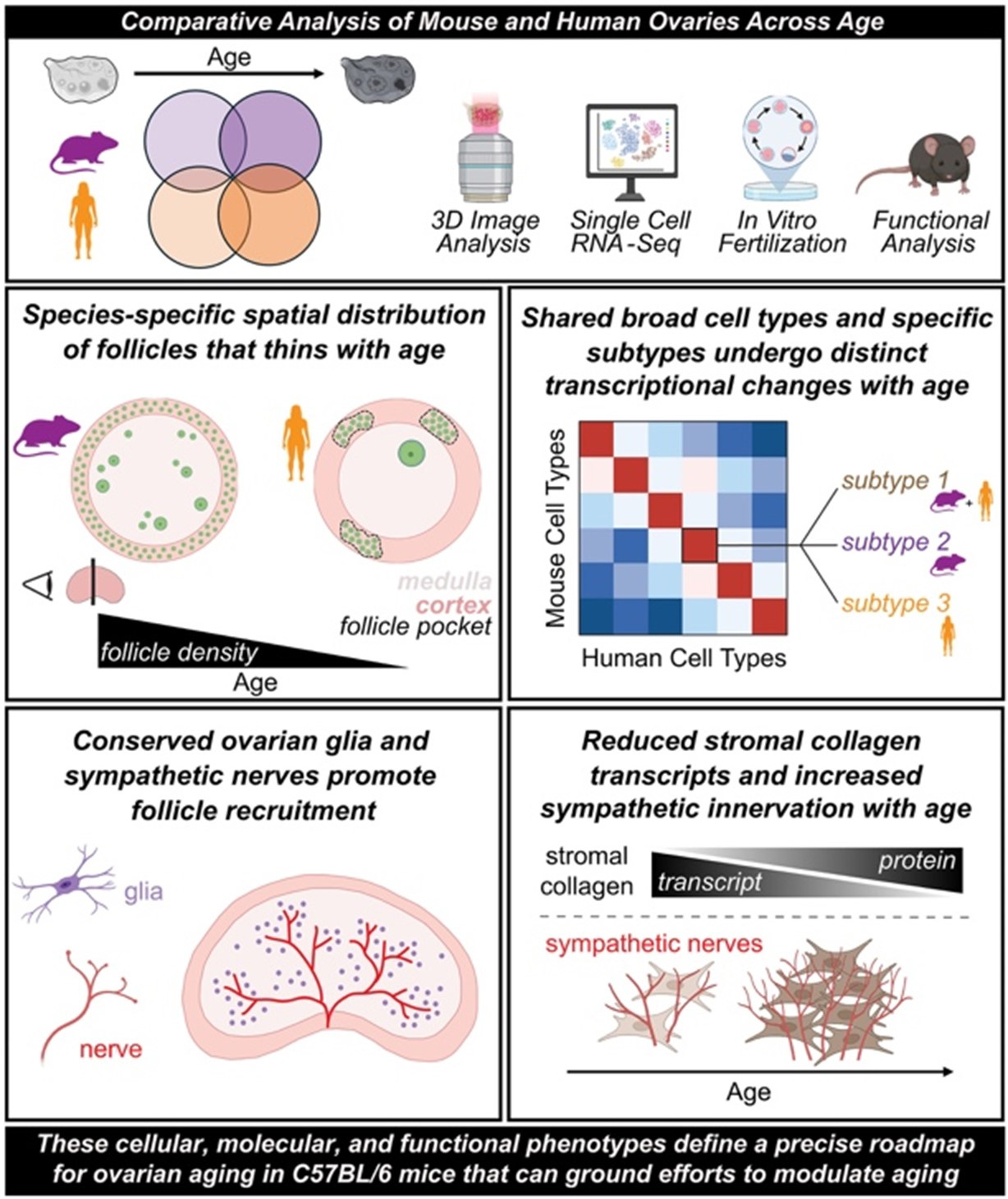
Specifically, the authors compared ovaries between the two species by using three-dimensional imaging, single-cell transcriptomics, and functional studies. In mice, they recorded declining follicle numbers and oocyte competence during aging. In human ovaries they studied demonstrated cortical follicle pockets and decreases in density.
Without going into detail, this study revealed probably more similarity between mouse and humans than expected in form of conserved cellular specialization. That included sympathetic nerves and glia and species-specific dynamics of follicle depletion with age, oocyte maturation, and stromal remodeling. This is important information, validating mouse models for many more future studies.
REFERENCES
Sen A, Hammes SR. Mol Endocrinol 2010;24(7):1393-1403
Gaylord et al., Science 2025;390(6778): DOI: 10.1126/science.adx0659
NEWLY APPROVED AND REGISTERED CLINICAL TRIALS AT THE CHR - READY FOR ENROLLMENT
Please call our registration desk at (212) 994 4400 if you or a friend is interested in further information.